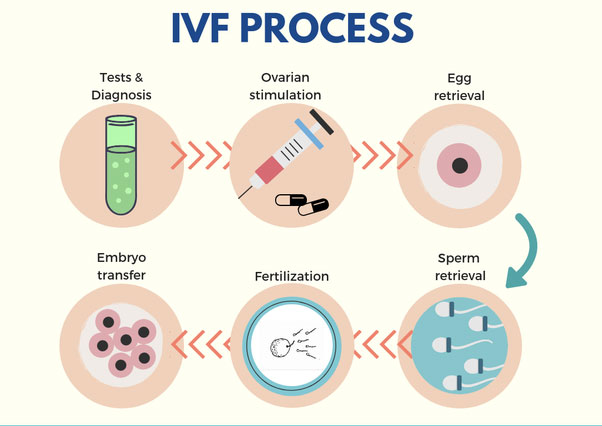
IVF process in 2020 step by step

Infertility: An Overview
February 17, 2020
IVF diet to boost success rate of IVF treatment
March 31, 2020This fact sheet is for someone who is considering or is about to start treatment with IVF (In Vitro Fertilization). It helps explain the overall IVF treatment procedure and discusses what is going on in the lab during the IVF cycle.
You decided to begin IVF treatment–so exactly what happens before, during and after IVF treatment?
IVF process step-by-step
What’s the IVF?
IVF stands for In vitro fertilization–which actually means’ glass fertilization.’ The name derives from the fact that, throughout the early days, the fertilization of eggs with sperm outside of the body used to be done in glass test tubes. The term IVF is now widely used to mean the entire pregnancy-creation treatment process in this way.
Does IVF suitable for me?
IVF can be the right treatment choice for couples who have trouble getting pregnant or who can not naturally establish a pregnancy. Whether infertility or low fertility, because the woman is unable to produce suitable eggs or the man, can not produce suitable sperm or a combination of both, there are different ways to increase the chances of a successful pregnancy through IVF by controlling the body’s medication systems and improving the biological processes in the laboratory.
Step 1: Stimulating egg development
Normally, a woman’s ovaries release a single mature egg every month, but in IVF treatment, we stimulate the ovaries to develop more follicles (which contain eggs) to produce a larger number of eggs. This means that there is a greater chance of transferring a healthy embryo back into the uterus.
Hormones:
In a natural cycle, follicle growth is stimulated by a hormone called the follicle-stimulating hormone (FSH). When the follicle is mature, another hormone called the luteinizing hormone (LH) releases the egg from the follicle (ovulation).
In the IVF cycle, we use artificial versions of FSH and LH to stimulate your ovaries to produce multiple follicles and also to control the timing of egg release (ovulation). This process is called’ controlled ovarian hyperstimulation’ (COHS). Medications are also used to switch off or reduce your own hormone signals and prevent them from disrupting the process.
You may be asked to take these hormones in a variety of ways, such as daily nasal spray or injections. FSH is typically a daily injection that is given to you by your IVF specialist.
Ultrasound monitoring:
We monitor the reaction of your ovaries and the development of follicles with ultrasound scans soon after treatment with FSH has begun. The ultrasound technique involves putting the probe gently into the vagina. Normally, this is painless and only takes a few minutes. The results of the scans will allow the doctor to adjust your medication, if necessary, to improve the development of the follicle. We may also test your blood to monitor the levels of Estrogen, or oestrogen (a follicle-producing hormone).
Occasionally this stimulation treatment has to be stopped and your treatment has to be postponed if the ovary doesn’t respond or seems to over-respond.
Step 2: Collecting eggs
The trigger:
When the ultrasound scan indicates that a number of follicles have attained a 17 mm diameter, we manage another ‘ trigger ‘ hormone that allows the eggs mature and release by imitating the LH surge that triggers ovulation in a normal menstrual cycle. The trigger may be administered through injection or as a nasal spray. You will have a procedure to collect the eggs 36 hours after the trigger is injected or sprayed before the eggs are naturally released from the follicles. This procedure is called egg pick-up (EPU) or egg retrieval.
Egg pick-up procedure:
The trigger is typically given late in the evening and you’ll get a meeting about 36 hours later for your EPU. Your IVF specialist will give you specific instructions on when and when to use the trigger to stop the stimulation medicines.
Before your egg collection procedure, you must not eat or drink for six hours. You will be asked to come about an hour before the time of your procedure to the IVF India Care, where you will be talking to one of our IVF nurses or Dr. Sumita Prabhakar. Our friendly IVFstaff will prepare you for the egg collection and do the admission paperwork.
EPUs may be performed under local anesthesia or sedation. You’ll be advised by your fertility doctor which is safest for you. If you have sedation, just before the procedure, you’ll meet the anesthetist, who will sedate you for about 30 minutes.
Using the ultrasound probe (as used during scanning) to guide a fine needle into the follicles we collect your eggs via your vagina. The follicles are drained by suction and flushing, and a doctor identifies and isolates the eggs from the contents of the follicles.
The nurses will take care of you when the procedure is over and the nurses at the IVF India Care fertility center will tell you how many eggs are collected.
Most people are ready to leave the clinic within 1-2 hours of collecting eggs. You’ll need someone to collect you from the hospital, as you’re not supposed to drive for 24 hours and you’re supposed to rest the rest of the day.
Meanwhile, your eggs are transferred into the IVF lab and stored 3 to 5 hours later in a cultivated medium prepared for sperm insemination.
Step 3: Collecting the sperm
The man will be asked to produce a sample of semen around the time of the collection of the eggs. The clinic has a private room for this purpose. Alternatively, if you reside at the IVF India Care within an hour’s travel time, the semen sample may be collected at home and sent to the clinic for the scheduled time. We suggest that the man not ejaculate between two and seven days before making the sample.
In situations where the man can not be available to produce a sample of fresh semen, we may plan to freeze a sample before collecting the eggs.
We may also arrange for donor sperm if needed. Please discuss this with your IVF doctor and nurse coordinator before starting your IVF treatment.
Step 4: In vitro fertilization and embryo culture Insemination:
Once a semen sample (or a sample of frozen sperm) has been collected by the laboratory, scientists separate normal swimming sperm from the semen.
For normal IVF, this formulated sperm is often used to inseminate the eggs, leaving them overnight in a culture dish. In order to have a better possibility that the eggs will be fertilized by this process, we need to have a large number of normal sperm.
Where the sperm count is too low for the regular IVF, or not of acceptable quality, one approach called the ‘ ICSI ‘ ‘intra-cytoplasmic sperm injection’ can be used, where one single sperm is inserted in every egg.
Fertilization check:
Depending on the method of insemination we use, the next day we will test the eggs under a microscope to see if they have fertilized. If an egg has fertilized, the male and female genetic material is evident in the egg as two spherical bodies.
At this point (Day 1), our scientist will be contacting you to let you know the results of your fertilization. Fertilization fails for about 5 percent of patients who have received eggs. This is sometimes due to an unexpected problem found with the eggs or sperm, but there is sometimes no obvious reason.
Development of embryos:
The fertilized egg is a single cell that then begins to divide. By day 3 the majority of embryos are between 5 and 8 cells. The cell numbers increase from day 3 onwards, and the cells begin to rearrange themselves, starting to differentiate into different types. Some of the embryos will attain a stage of development called a blastocyst by day 5. Each day, a scientist tests the embryos and measures and documents their progress and quality.
Step 5: Embryo transfer and freezing:
Embryo transfer:
at IVF India Care, we usually transfer embryos on day 5 after fertilization, when they’re at the blastocyst stage. If your embryos need to be transferred sooner, your IVF specialist will advise you. In order to transfer the embryo, a thin plastic tube called a transfer catheter places the embryo(s) in the uterus.
A speculum has been inserted into the vagina (such as a pap smear) and the cervix (the entrance to the womb) is situated. A scientist uses a syringe to extract and implant the embryo(s) at the tip of the catheter. The catheter is passed into the uterus through the cervix and the embryo(s) into the womb.
The procedure only takes a few minutes and generally does not require an anesthetic. You will be asked to provide a full bladder so that the clinician can use an abdominal ultrasonic scan to show the transfer of the embryo.
Embryo Freezing:
If you have embryos of higher quality than you need, they can be preserved for use in the future. Both embryos are grown in the lab until day 6 in case any more embryos at this stage can be cryopreserved.
In some patients, immediately after the EPU, a fresh embryo transfer is not planned. Alternatively, the clinician may ask the laboratory to freeze all appropriate embryos of good quality at the blastocyst stage (days 5 and 6) with the intention to thaw and transfer an embryo in a subsequent frozen embryo transfer period (FET). If we think this is the right idea for you, your IVF doctor will discuss it with you in advance.
Step 6: Pregnancy test and follow-up
Blood test for pregnancy 11-14 days after the transfer of the embryo. The blood test measures the hormone human Chorionic Gonadotropin (hCG), which is produced by early pregnancy. Wait until the day you are told to have your check, as the hormones used during the process will lead to false readings if you check too soon.
Before their pregnancy test, some women experience bleeding or spotting. This is not usually a phase and it is vital that you continue to take your prescription medicine until you have spoken to your Nurse Coordinator or Fertility Specialist.
The doctor can repeat blood tests if the test is positive to validate the result. If you’re on medicine to protect the endometrial lining, it’s vital you keep on taking it.
Contact IVF India CARE Fertility Center
IVF India CARE Fertility Center’s welcoming and knowledgeable team is happy to answer any other questions you might have about the IVF phase.